When your child is newly diagnosed with cancer, information comes at you in a way that doesn’t match the moment you’re in.
Everything feels like a dream you haven’t woken up from and then someone you don’t really know—but also feel like you’ve known forever—says, “They’ll need a central line.”
A line?
I remember hearing that and nodding, already understanding that this wasn’t really a decision to make. What choice did we have? Then Andrea, our child life specialist, placed a small piece of plastic in my hand and said, “This is what the port looks like.”

I stared at it and wondered how she could be wearing such whimsical pants—gauchos covered in elephants—while explaining that they would implant this just below my son’s clavicle.
It made me sick. He was only six years old, and now this thing would live inside his body. It felt egregious. I had grown this precious child cell by cell, and now science was going to implant a piece of plastic into him?
But like everything else in those first days after diagnosis, I just nodded, we signed the consents, and waited for surgery to be over. The team explained everything carefully. My body absorbed it; my mind did not.
If you’re here because someone just told you your child is getting a central line and your brain went a little fuzzy, this post is for you.
· · ·
So… What Is a Central Line?
A central line is a special kind of IV that goes into a large vein near the heart. That’s the medical definition, anyway.
In real life, it’s simply a stable access point- a reliable way for treatment to happen.
· · ·
Why Central Lines Are Used in Cancer Treatment
Chemotherapy is hard on peripheral veins—the hands, the elbow crease, the usual IV spots. It can injure these veins and make them unusable. During treatment, blood draws are frequent, as are medications, fluids, and transfusions. All this can add up quickly, taxing those tender peripheral veins. Over time, those veins can become irritated or worse, stop working. This often means more attempts at access—something no child needs more of.
A central line allows the process to happen in a reliable way, not reliant on IV access.
· · ·
The Main Types of Central Lines You’re Likely to Hear About
Different hospitals use different types of central lines, but these are the most common central lines in pediatric oncology. You don’t need to memorize this—just enough to recognize the words when they come up.
Ports

A port is a small disc placed completely under the skin, usually in the chest, with a catheter that goes into a large vein. The “catheter” is like a long, flexible straw. When it’s not being used, you can see a small raised area under the skin.
To access a port, a special needle goes through a thin layer of skin and rests in the reservoir. From there, medicine can be pushed through the needle and will flow through the catheter and empty into the bloodstream.
Numbing cream (Emla cream) is often used to help with the discomfort of a port access. Sometimes it works, sometimes it doesn’t. Either way, it takes time—for kids and parents alike—to get used to the process.
Ports are common for longer treatment plans. They are easy to manage, day-to-day, once things settle in—less visible, less daily care at home. You can still swim or shower, for example, which is not the case for other line options. Fever Protocol, which I discuss below, is an issue with a port, and all other central lines.
One small “port life” detail: ports are often heparin-locked to help prevent clotting—usually about once a month when they aren’t being used—but the exact timing (and whether your center uses heparin or saline) depends on your hospital’s protocol, so your team will tell you what applies to your child.
PICC Lines

A PICC line is placed in a vein in the arm and threaded toward the heart, with tubing that stays outside the body. PICC lines are put in under sedation and require more daily attention than a port.
They’re often used when treatment timelines are shorter or when a port isn’t the right fit. They are also sometimes used when multiple access points are needed in addition to the port. Such as during a T-cell aphaeresis process during CAR T-cell therapy.
Because the access point is always exposed, they do restrict swimming and require special care for showering/bathing.
Broviac / Hickman Lines
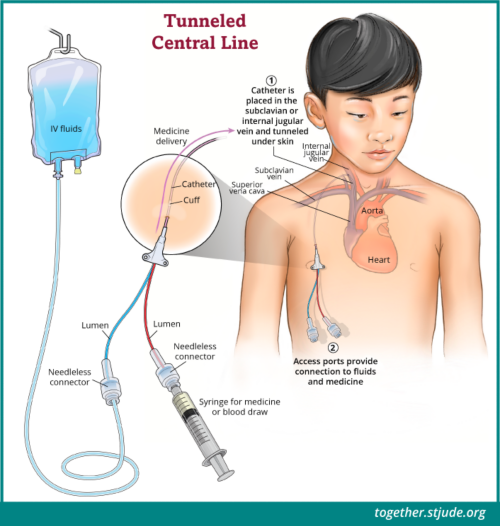
These are tunneled lines placed in the chest with external tubing. They’re often used for very intensive or prolonged treatment. Similar to a PICC line, they can also be used in circumstances where more access points are needed, commonly during a Bone Marrow Transplant/ Stem Cell Transplant.
Similar limitations to the PICC line are present with the Broviac/Hickman.
PowerWand (Situational, Less Common)

The PowerWand isn’t a long-term central line, but I mention it because during CAR-T therapy it made a real difference for us during the apheresis process.
It’s not offered everywhere, but it’s worth knowing it exists. It’s essentially a high-flow IV—used when more flow is needed than a standard IV can handle. It is put in with the patient awake, removing the added sedation needed for a PICC line. Anecdotally, it appears less painful to remove than a PICC.
You can read about our experience with PowerWands here.
· · ·
A Note About Fever and Infection (Just the Basics)
One thing that comes up pretty quickly once a central line is in place is how seriously fevers are taken. Fever protocol is something you will become very familiar with.
That’s because a central line goes straight into a large vein, which means infections in the bloodstream can spread quickly. A fever of any origin usually triggers a protocol—going urgently to the ER, blood cultures, antibiotics, observation—not because something is definitely wrong, but because it’s better to move fast than to wait and see. Never use fever reducing medicine until you have spoken with your care team.
Fever protocol looks different at different facilities, so I won’t try to lay out exact steps here. Your provider will tell you their guidelines and will probably give you something simple to reference, like a fridge magnet, with the temperatures you need to watch for and who to call.
My main recommendation here is very practical: get one thermometer you trust and only use that one. Don’t have two or three different ones floating around the house and try each of them—you will get three different readings, and hand to God, you will lose your mind. Also, resist the urge to take your child’s temperature every five minutes. Trust me.
Click here to see the thermometer I recommend. Highly recommend this or one similar as the display illuminates with color based on the temperature which makes a middle of the night read much easier.
Fever protocol will become a second language to you. And by that I mean that once this hell ride is over and your child gets their port out- the first time they get a fever, port-free, you will cry tears of joy at how amazing their sweaty forehead feels.
· · ·
One Last Thing
When they first told me about the port, I panicked at the idea that Beaudin would have an implanted device in his perfect little body. Something foreign, living inside him.
But over time, something shifted.
I found myself feeling quietly thankful for it. Even fond of it, in a way that surprised me. In the same odd, childlike way I once believed my stuffed animals had feelings and opinions, this small port began to feel like it had a job—and a personality. Like it knew what it was there to do. Like it was doing something tender: protecting Beau, bringing him the medicine he needed, helping his body through something impossibly hard.
Every cell of my body resisted the child life specialist when she told me they would implant him with a port.
And three and a half years later, every cell of my body ached with gratitude when it was finally removed. What once made me feel like my child was being invaded had become something I trusted completely. Letting it go felt like a real goodbye—the kind you give to a stuffed animal you long believed had been keeping watch.
I wrote about the port removal here:
I’m not a doctor, and this is not medical advice. This is simply our experience and information from the internet. Please talk with your care team before making any medical decisions.




Leave a Reply